Clinical Significance of Extreme Elevation of the Erythrocyte Sedimentation Rate: Diagnoses and Survival in 681 Patients in a Portuguese Hospital.
DOI:
https://doi.org/10.24950/rspmi.2579Palavras-chave:
Blood Sedimentation, MortalityResumo
Introduction: We aimed to study the association between extreme erythrocyte sedimentation rate (ESR) elevations (>100 mm/h), and the distribution of disease categories, diseases, age, sex, C-reactive protein levels and five-year survival.
Methods: a retrospective study of all patients with extreme ESR values examined at a Portuguese hospital, from January 1, 2008, through December 31, 2012. Independent variables included disease categories, subcategories, age, sex, and CRP level. Living status and date of death were determined
using the Portuguese Electronic Prescription System.
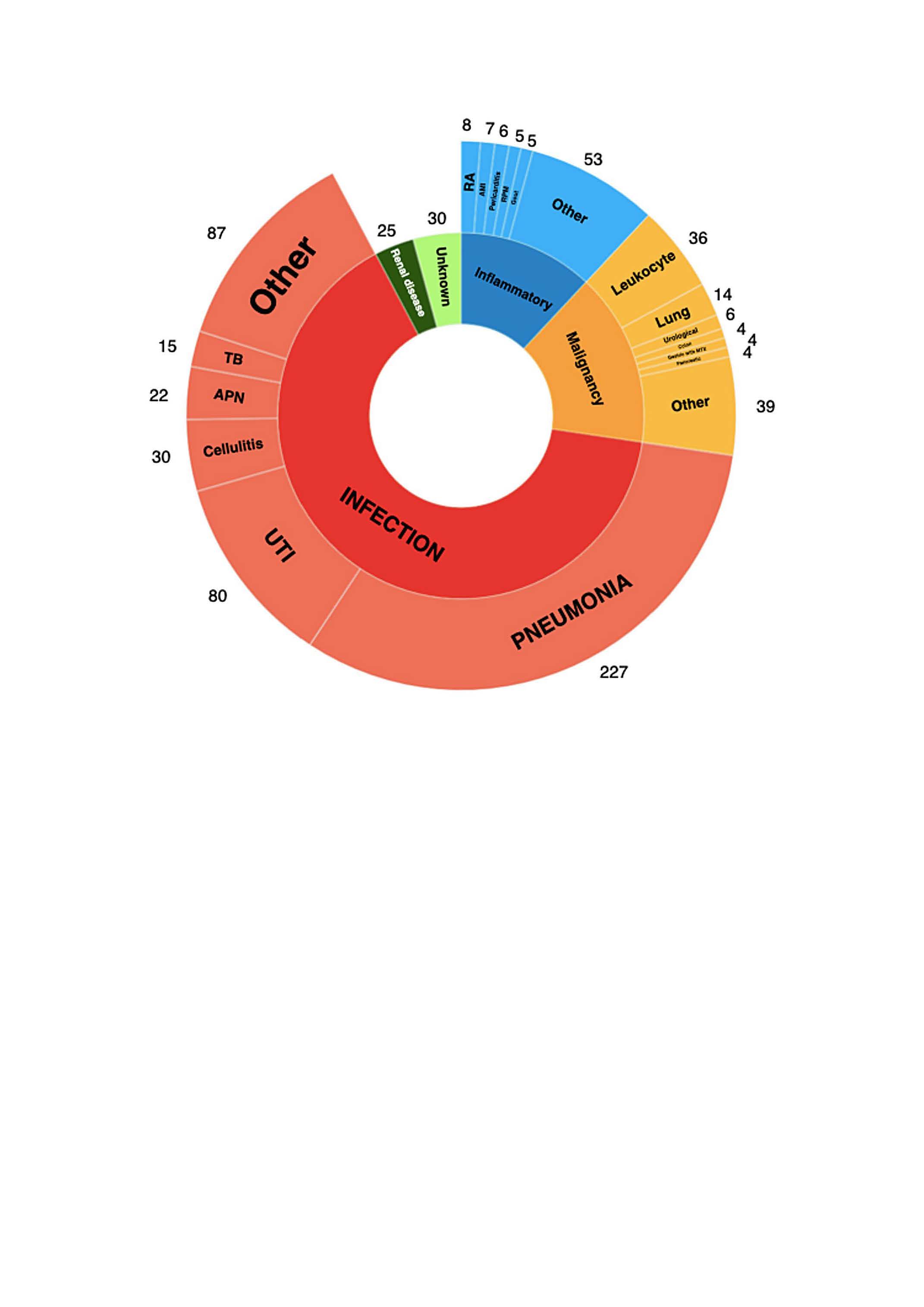
Results: An ESR above 100 mm/h was found in 681 patients (1.5% of all determinations). The leading diagnosis category was infection (461, 65.1%), followed by malignancy (107, 15.1%), and inflammatory/autoimmune (85, 12.0%). The most
prevalent disease was pneumonia (227, 33.3% of all patients). Infection was less likely in outpatients (20.7%), as was malignancy in females (11.4%). Five-year mortality was 70.3%, higher in patients with malignancy (83%) and lower in patients with inflammatory/autoimmune disease (45.9%).
Conclusion: We found that almost all patients with an extreme ESR elevation have an identifiable etiology, with infection observed in nearly two-thirds and pneumonia being the most common disease in one-third of all patients. Infection was less likely in outpatients, as was malignancy in females. The ESR and CRP levels correlated poorly in patients with extremely elevated ESRs. The five-year mortality rate was 70.3%, with survival being significantly lower in patients with malignancy, and higher in those with inflammatory/autoimmune disease. These findings may enhance the diagnostic and prognostic evaluation of patients with extreme elevations in ESR.
Downloads
Referências
Ropes MW, Rossmeisl E, Bauer W. The relationship between ESR and plasma proteins. J Clin Invest. 1939;18:791-8. doi: 10.1172/JCI101096.
Bedell SE, Bush BT. Erythrocyte Sedimentation Rate. From Folklore to Facts. Am J Med. 1985;78:1001-9. doi: 10.1016/0002-9343(85)90224-4.
Fincher RM, Page MI. Clinical significance of extreme elevation of the erythrocyte sedimentation rate. Arch Intern Med. 1986;146:1581-3.
Zacharski LR, Kyle RA. Significance of extreme elevation of erythrocyte sedimentation rate. JAMA. 1967;202:264-6.
Ford MJ, A. IJ, Parrish FM, Allan NC, Horn DB, Munro JF. The significance of gross elevations of the erythrocyte sedimen- tation rate in a general medical unit. Eur J Clin Invest. 1979;9:191-4. doi: 10.1111/j.1365-2362.1979.tb00922.x.
Daniels LM, Tosh PK, Fiala JA, Schleck CD, Mandrekar JN, Beckman TJ. Extremely Elevated Erythrocyte Sedimentation Rates: Associations With Patients' Diagnoses, Demographic Characteristics, and Comorbidities. Mayo Clin Proc. 2017;92:1636-43. doi:10.1016/j.mayocp.2017.07.018
Wyler DJ. Diagnostic implications of markedly elevated erythrocyte sedimentation rate: a reevaluation. South Med J. 1977;70(12):1428-30. doi: 10.1097/00007611-197712000-00015.
Alvarenga MJ, Loureiro MC, Van-Dunen F, Mota L, Murinello A. Causas de velocidade de sedimentação extremamente elevada. Rev Port Doenças Infecc. 1995;18:129-33.
Yousuf M, Akhter J, Al-Khairy K, Al-Saadan MA, Bin-Salih S. Extremely elevated erythrocyte sedimentation rate. Etiology at a tertiary care center in Saudi Arabia. Saudi Med J. 2010;31:1227-31.
Wyler DJ. Diagnostic implications of markedly elevated eryth- rocyte sedimentation rate: a reevaluation. South Med J. 1977;70:1428-30. doi: 10.1097/00007611-197712000-00015.
Brigden ML. Clinical Utility of the Erythrocyte Sedimentation Rate. Am Fam Physician. 1999;60:1443-50.
Osei-Bimpong A, Meek JH, Lewis SM. ESR or CRP? A comparison of their clinical utility. Hematology. 2007;12:353- 7. doi: 10.1080/10245330701340734.
Tsao CW, Lyass A, Enserro D, Larson MD, Ho JE, Kizer JR, et al. Temporal trends in the incidence of and mortality associated with heart failure with preserved and reduced ejection fraction. JACC Heart Fail. 2018;6:678-85. doi:10.1016/j.jchf.2018.03.006
Kann AE, Jepsen P, Madsen LG, West J, Askgaard J. Cause-specific mortality in patients with alcohol-related liver disease in Denmark: a population-based study. Lancet Gastroenterol Hepatol. 2023;8:1028-34. doi:10.1016/S2468-1253(23)00192-9
American Cancer Society. Cancer Facts & Figures 2023. Atlanta: ACS; 2023.
Costenbader KH, Chibnik LB, Schur PH. Discordance between erythrocyte sedimentation rate and C-reactive protein measurements: clinical significance. Clin Exp Rheumatol. 2007;25:746-9.
Feldman M, Aziz B, Kang GN, Opondo MA, Belz RK, Sellers C. C-reactive protein and erythrocyte sedimentation rate discordance: frequency and causes in adults. Transl Res. 2013;161:37-43. doi: 10.1016/j.trsl.2012.07.006.
Downloads
Publicado
Como Citar
Edição
Secção
Categorias
Licença
Direitos de Autor (c) 2025 Medicina Interna

Este trabalho encontra-se publicado com a Creative Commons Atribuição-NãoComercial 4.0.








